Chloroquine resistant Plasmodium vivax review
Systematic review of the extent of chloroquine resistant P. vivax and the different methodologies used to quantify therapeutic efficacy
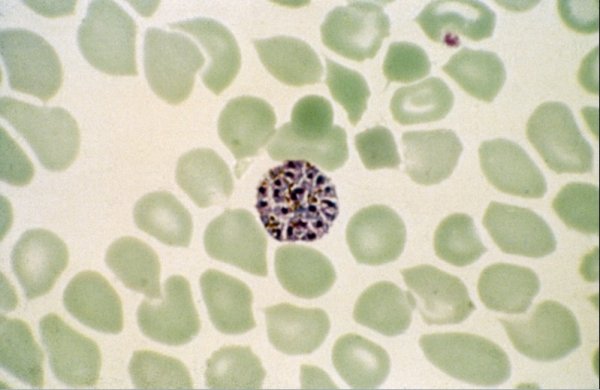
One of the major threats to malaria control and elimination efforts is the ongoing spread and emergence of resistance towards commonly used antimalarial drugs to treat P. falciparum and P. vivax infections. Whilst our understanding of drug resistant P. falciparum is quite well understood, the extent and nature of resistance in P. vivax parasites is for the most part is unknown. One of the reasons for this is the difficulty in interpreting P. vivax clinical efficacy studies. Unlike P. falciparum, P. vivax forms hypnozoite liver stages that can lie dormant in the liver for many years before re-emerging. Hence recurrent parasitaemia following treatment can represent recrudescence (the same parasite), reinfection (a new infection) or relapses (an infection arising from the dormant liver stage). Current genotyping methods are unable to distinguish between these patient responses.
A recent systematic review of literature illustrates the diversity of methodologies that have been used to quantify therapeutic efficacy and summarizes the current geographical extent and level of evidence for reduced P. vivax susceptibility to chloroquine. The review highlights that chloroquine resistance has been underappreciated, with evidence for reduced susceptibility in many areas where vivax is endemic.
-
There was marked heterogeneity in the design of the clinical studies assessing the efficacy of chloroquine towards P. vivax.
-
Patients receiving chloroquine plus primaquine had an equivalent or lower risk of P. vivax recurrence by day 28 compared with patients receiving chloroquine alone.
-
Overall P. vivax was defined as chloroquine resistant for more than half of the 122 sites where efficacy could be assessed.
-
Delayed parasite clearance was predictive of early recurrence.
A systematic search of Medline, Web of Science, Embase and the Cochrane Database of Systematic Reviews was conducted. You can download a full publication library of the clinical trial references from 1960-2013.
Chloroquine resistance (CQR) was defined as follows:
- CQR Category 1 - >10% recurrences by day 28, the lower 95% confidence interval on this estimate being >5%, irrespective of confirmation of adequate blood chloroquine concentration. Occasional breakthrough recurrences do occur within 28 days of chloroquine treatment, but a risk greater than 10% in a large enough sample is highly suggestive of resistance.
- CQR Category 2 - Confirmation of recurrences within 28 days in the presence of whole blood concentrations greater than 100nM. Parasite growth in the presence of high blood concentrations of the drug confirms chloroquine resistance.
- CQR Category 3 - >5% recurrences by day 28, with the lower 95% confidence of this estimate lying below 5%, irrespective of confirmation of adequate blood chloroquine concentration. This represents potential evidence of CQR, but may reflect other factors such as poor drug absorption or quality.
- Chloroquine Sensitive CQS - confirmation of sensitivity requires all of the following: patients enrolled following a symptomatic clinical illness, less than 5% recurrences by day 28, no administration of primaquine before day 28, and a sample size of at least 10 patients.
A total of 129 clinical trials were included in the analyses.
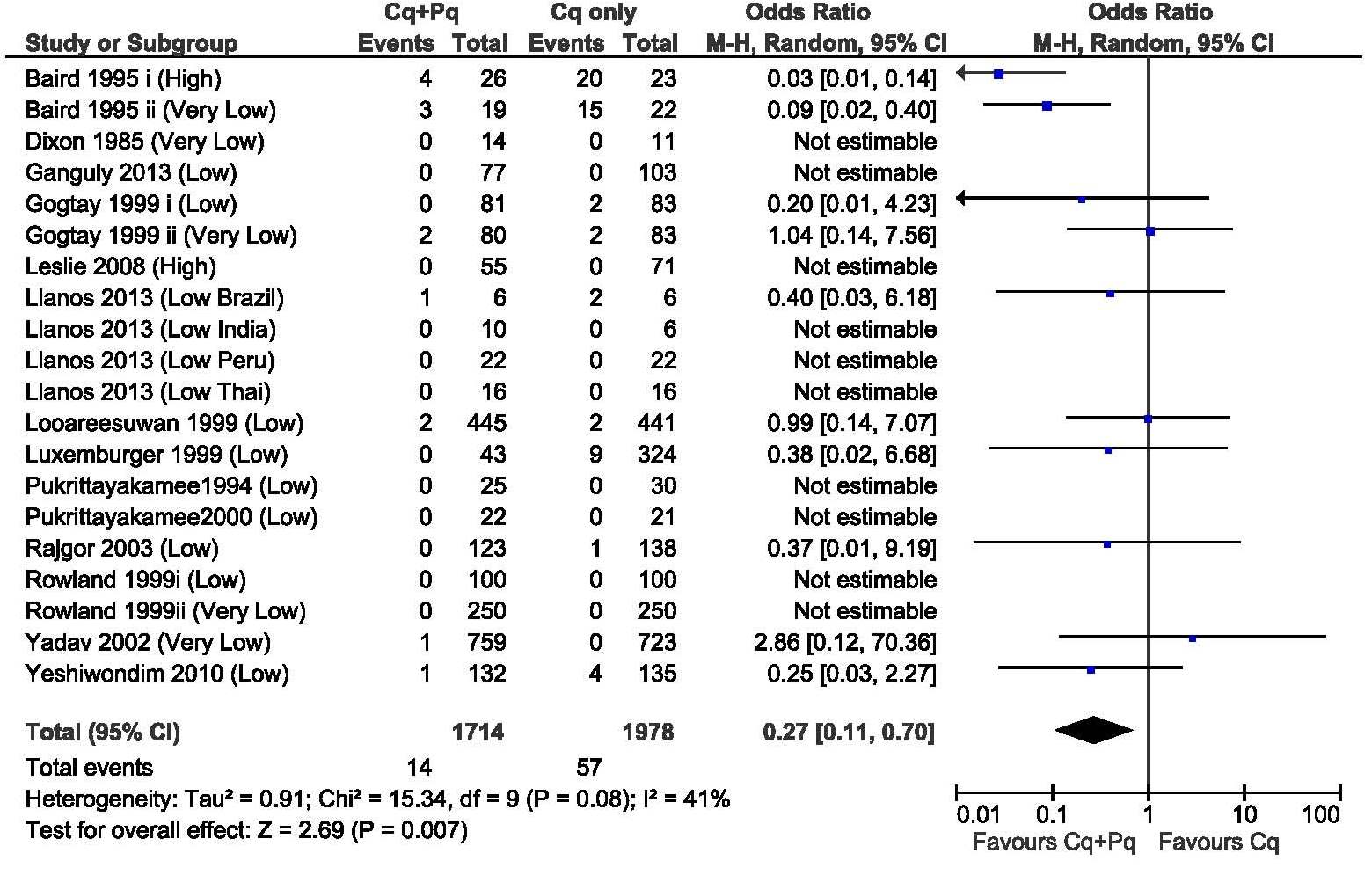
Figure 1 shows the risk of recurrence at day 28 for patients treated with chloroquine alone and for patients treated with chloroquine and primaquine. A total of 14 studies included patients recruited into comparative studies of chloroquine monotherapy and chloroquine plus primaquine administered at the start of treatment. In all but one of these studies patients receiving chloroquine plus primaquine had an equivalent or lower risk of P. vivax recurrence by day 28. The overall Odds Ratio (OR) was 0.27 (95%CI 0.11-0.70; p=0.007).
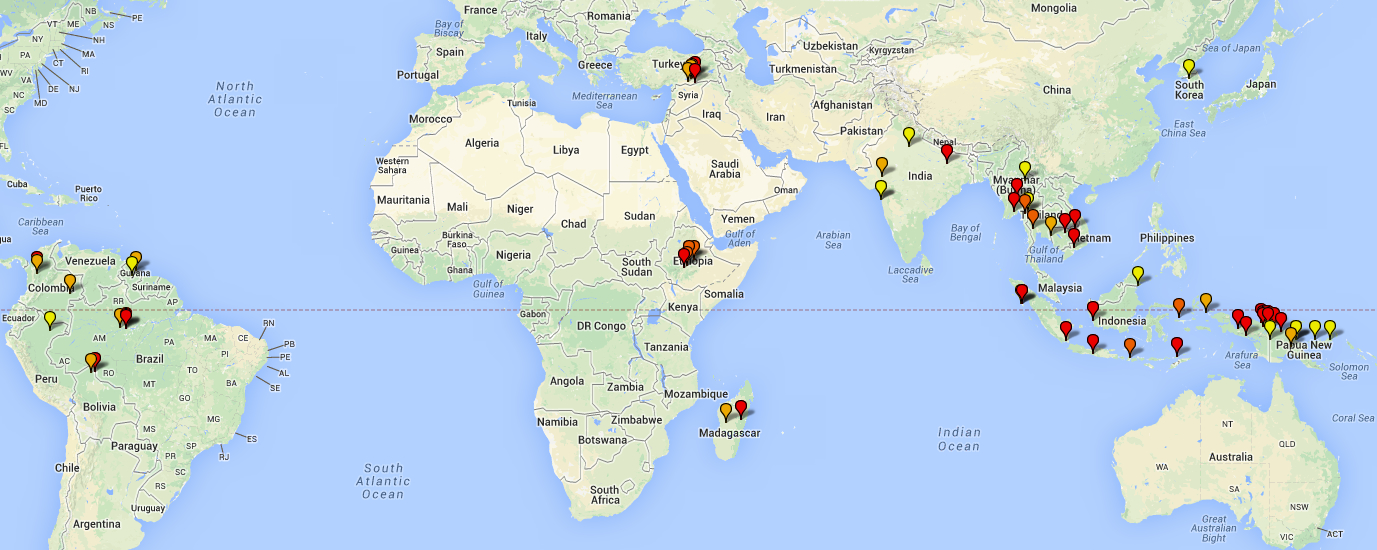
The location of study sites with documented chloroquine resistance and chloroquine sensitive P. vivax is shown in Figure 2a and for chloroquine sensitive sites in Figure 2b below. Estimates for chloroquine sensitivity derived from 112 sites. In 50.9% of the sites estimates P. vivax were categorized as resistant. You can download an excel file of the extracted data from the P. vivax antimalarial efficacy study sites.
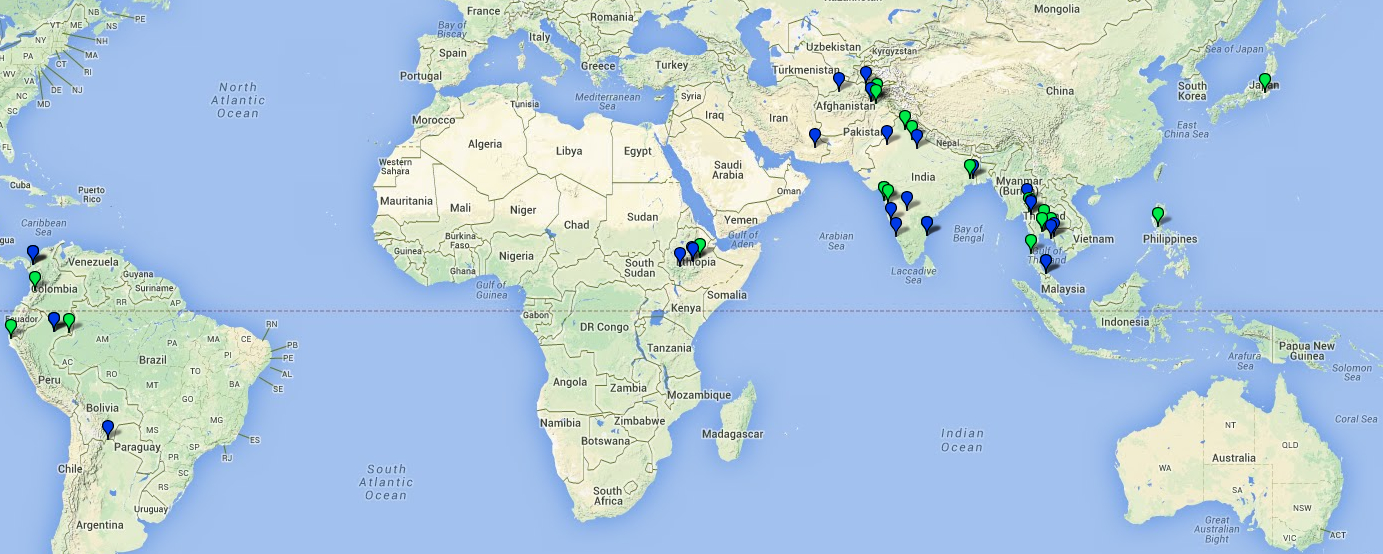
Fig. 2a legend Red icons = Category 1; Dark Orange = Category 2; Light Orange = Category 3; Yellow = case reports.
Fig. 2b legend Green icons = conducted prior to 2008; Blue icons = conducted between 2008-2014.
Figure 3 shows the proportion of patients with parasites in the peripheral blood stream on day 2 and 3 divided by CQR and CQS based on day 28 recurrence. Site estimates categorized as CQR had significant higher proportions of patients that were parasitaemic on day 2 and 3 compared to those categorized as CQS.
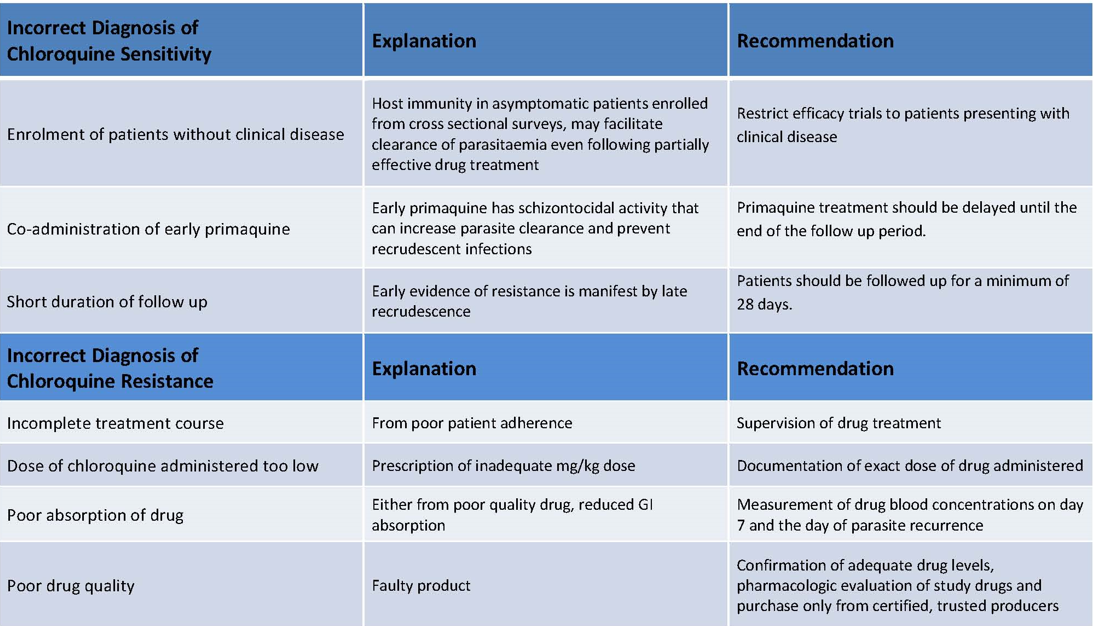
CQR P. vivax poses a significant threat to malaria endemic communities. Enhanced monitoring of P. vivax drug efficacy is needed to adapt treatment policy accordingly. This will require standardised methodologies and the development of novel tools for the more precise quantification of drug efficacy. Figure 4 shows the common causes for misdiagnosis of chloroquine sensitivity and chloroquine resistant P. vivax.
WWARN provides an example of a protocol template for researchers, which we believe addresses the main challenges of P. vivax efficacy monitoring and can be adapted to site specific needs. Download the WHO manual for therapeutic efficacy monitoring, including protocols for the study of P. vivax.
View the abstract: Price RN, von Seidlein L, Valecha N, et al. The global extent of chloroquine resistant plasmodium vivax: a systematic review and meta-analysis. Lancet Infectious Diseases; DOI S1473-3099(14)70855-2.