Malaria treatments deemed safe and effective to use on pregnant women
Two new studies, published today in the New England Journal of Medicine, announce the results from clinical trials investigating the safety and efficacy of antimalarial medicines, currently used in the wider population, on pregnant women.
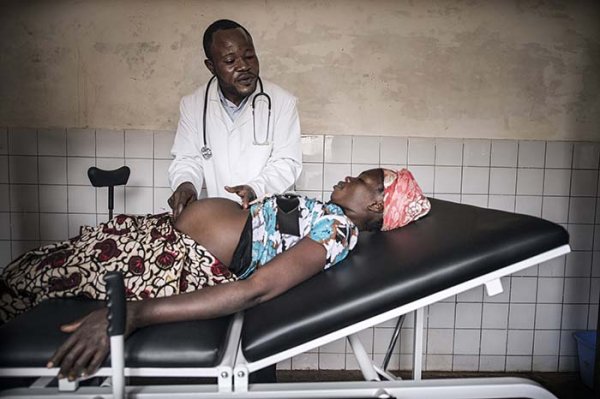
Malaria infection during pregnancy is a major health concern to both the mother and unborn child. It is thought to be responsible for the deaths of 100,000 infants in Africa alone each year. Most people living in malaria endemic sub-Saharan Africa develop a certain level of immunity to the malaria parasite once they reach adulthood. However, during pregnancy this acquired immunity declines, making pregnant women more susceptible to the effects of malaria infection.
Due to ethical concerns, pregnant women are systematically excluded from clinical trials. This means there is very little information on the safety, efficacy and pharmacology of current antimalarials in pregnant women, especially in sub-Saharan Africa.
Two new studies published today in the New England Journal of Medicine announce the results from clinical trials investigating the safety and efficacy of antimalarial medicines, currently used in the wider population, on pregnant women.
The first of the papers, led by the University of California, San Francisco, explored the efficacy of dihydroartemisinin-piperaquine (DP) as a preventative measure against malaria infection in pregnant women. The current first line preventative treatment for malaria in pregnancy is sulphadoxine-pyrimethamine (SP), but widespread emergence of drug resistance against SP throughout the region has meant the drug is often failing to protect against malaria infection. The team compared treatment with SP against treatment with DP and found that, in general, DP was much more efficacious at preventing malaria infection in pregnant women.
“People are very cautious about giving drugs during pregnancy,” said Grant Dorsey, MD, PhD, professor of Medicine at UCSF and senior author of the first paper. “You don’t want to take any chances that it’s going to do something bad to the foetus or to the mother.”
The trial included 300 pregnant women in their second or third trimester. 40 per cent of women treated with SP were found to still have malaria parasites in their blood, compared to 17 per cent of those treated with DP on the same regimen. This figure dropped to 5 per cent when DP was used monthly. Moreover, none of the women on monthly DP became ill with malaria, while there were 41 episodes of malaria among the 106 women receiving SP. Further research needs to be undertaken to scope out the full safety profile of using DP during pregnancy.
The second study, led by the PREGACT (PREGnancy Artemisinin-based Combination Treatments) Study Group at the Institute of Tropical Medicine in Antwerp, compared the safety and efficacy of four artemisinin combination therapies at treating malaria infections in close to 3,500 pregnant women. Although there were some differences between all four treatments, the team concluded that each was safe and effective to treat malaria in pregnancy.
The women who took artermether-lumefantrine (AL) had the fewest complications, acceptable cure rates, but the shortest protection against re-infection. DP was the most effective treatment, with good safety and longer protection from re-infection after treatment.
“We hope that the use of these ACTs among pregnant women will now increase,” said Prof Umberto D’Alessandro, the study’s coordinating investigator, who is affiliated with the Antwerp Institute of Tropical Medicine (ITM), the Medical Research Council Unit The Gambia (MRCG) and the London School of Hygiene and Tropical Medicine (LSHTM). “These results provide strong support for the use of ACTs in the second and third trimester of pregnancy and will help African countries in either confirming or changing their treatment guidelines for pregnant women with malaria.”
These studies highlight the effectiveness of artemisinin combination therapies at treating uncomplicated malaria infection and the effectiveness of DP at preventing malaria in pregnant women, without evident safety concerns.
Prof Joel Tarning, Head of Pharmacokinetics at WWARN, contributed an editorial piece to the NEJM on both papers. “These papers clearly indicate artemisinin combination therapies can be safely and effectively used to treat and prevent malaria infection in pregnant women. However, prospective pharmacokinetic studies are still needed to determine the pharmacologic properties of these drugs to provide pregnant women with optimal treatments.”
WWARN and the Malaria in Pregnancy Consortium have recently joined forces to establish a malaria in pregnancy research programme within the WWARN data platform. These studies, published in NEJM, complement the work of this partnership that aims to develop a better understanding of the impact of resistance on the effectiveness of current prevention strategies, and help ensure that all pregnant women with malaria receive safe and effective malaria treatment.
Related studies:
- Tarning, J. 'Treatment of Malaria in Pregnancy' New England Journal of Medicine 2016; 374:981-982 March 10, 2016 DOI: 10.1056/NEJMe1601193
- Kakuru, A et al. 'Dihydroartemisinin–Piperaquine for the Prevention of Malaria in Pregnancy' New England Journal of Medicine 2016; 374:928-939March 10, 2016 DOI: 10.1056/NEJMoa1509150
- The PREGACT Study Group. 'Four Artemisinin-Based Treatments in African Pregnant Women with Malaria'. New England Journal of Medicine 2016; 374:913-927 March 10, 2016 DOI: 10.1056/NEJMoa1508606
