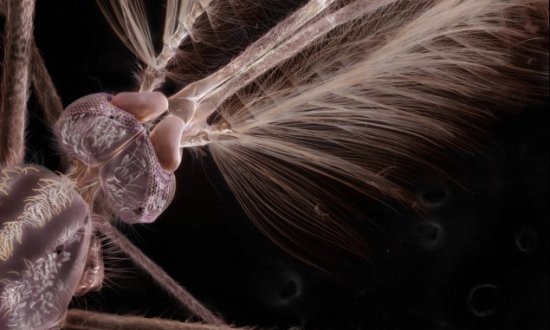
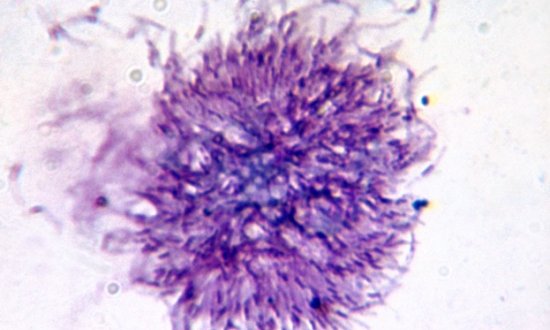
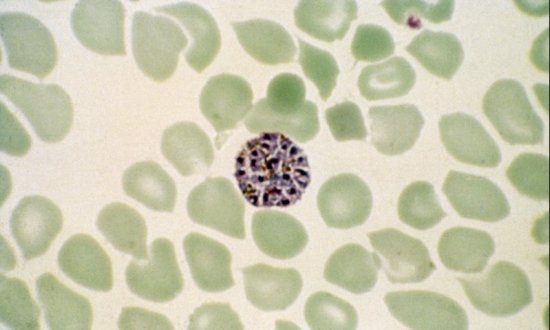
Malaria Drug Resistance
Malaria medicines are working well in many parts of the world, however, there is serious concern that malaria parasites are once again developing widespread resistance to antimalarial drugs.
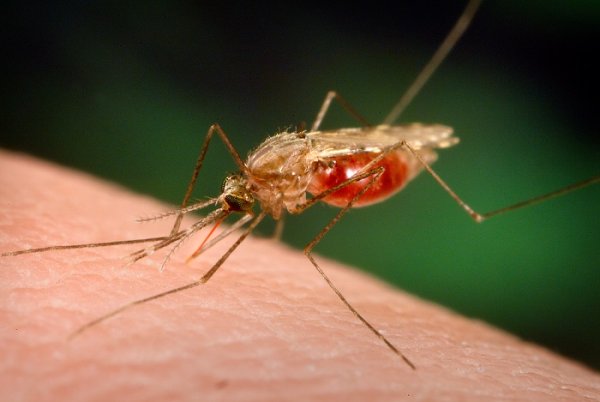
Malaria remains one of the most devastating infectious diseases with approximately 228 million infections and 405,000 deaths in 2018 – primarily children under the age of five in sub-Saharan Africa.
Plasmodium falciparum, the deadliest form of the malaria parasite, is responsible for the vast majority of the mortality and morbidity associated with malaria infection. Artemisinin Combination Therapies, or ACTs, are currently the frontline treatments against P. falciparum malaria. Although these treatments are working well in many parts of the world, there is serious concern that malaria parasites are once again developing widespread resistance to this vital treatment.
As the threat of antimalarial drug resistance grows, there is increasing pressure to sustain the efficacy of existing treatments, develop alternative treatments, as well putting in place preventative measures such as bednets.
Key drivers of antimalarial drug resistance
- Unusual genetic structure of malaria parasites in regions known for antimalarial drug resistance
- Counterfeit or substandard treatments
- Unregulated or poorly administered antimalarial drug use
- Artemisinin drug use without a complementary combination treatment, such as lumefantrine
Plasmodium vivax, is responsible for the majority of cases in the Americas (75%), while most P. vivax is found in Southeast Asia (53%). Plasmodium vivax presents different challenges to Plasmodium falciparum:
- It is difficult to detect as it circulates at low levels in the blood
- It can be infectious to mosquitoes even when the person has no symptoms
- It can lie dormant in a person’s liver, reawakening weeks to months after
- In many places, chloroquine treatment is no longer effective because of drug resistant P. vivax.
- There is a shortage of accurate diagnostics
What is the WWARN network doing to stop this?
- Facilitating Study Groups to generate pooled analyses to understand the efficacy and safety of antimalarials, incuding for sub-populations
- Advocating for better understanding of the impact of poor quality drugs on malaria control through the work of the Medicine Quality Group
- Designing data visualisation and mapping tools to track the spread of resistance - these can be used to inform government-lead surveillance strategies
- Developing freely available tools, resources and training courses to provide regional researchers with the knowledge and skills to generate high-quality antimalarial clinical data